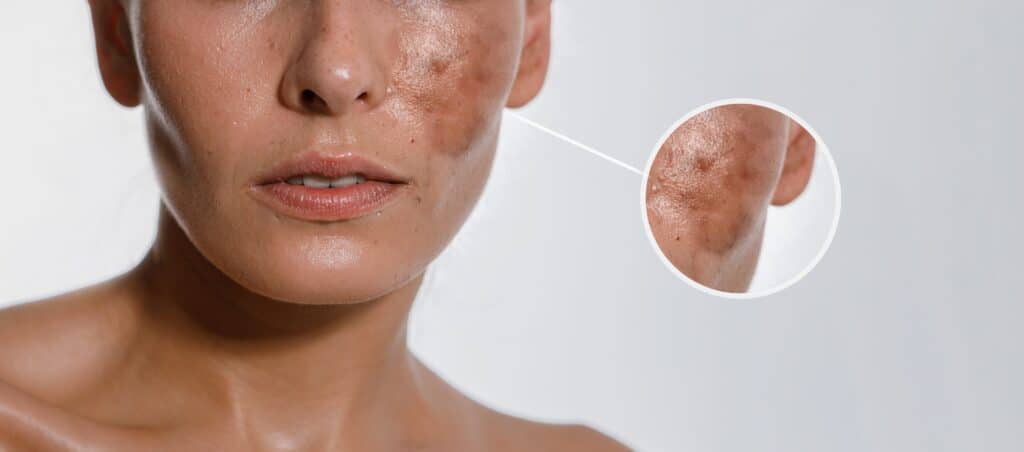
Acne vulgaris can be associated with hyperpigmentation, especially for individuals with skin of color. In fact, in patients with Fitzpatrick phototypes III-VI, acne is often accompanied by post-inflammatory hyperpigmentation (PIH) or acne-induced macular hyperpigmentation (AMH). For many, PIH is long-lasting and can have a significant impact on quality of life. One study of acne-induced PIH revealed that over half of the patients (65.2%) endured PIH for at least a year. For the other 22.3% of patients, PIH lasted for over five years.
Despite the multitude of acne treatments currently available, further research and effective tools for the treatment of AMH are limited. The condition, however, is a common one and there is an ongoing need for management strategies to help guide clinicians. Recently, a group of 10 board-certified dermatologists conducted a Delphi consensus to evaluate the best methods for managing AMH. They aimed to reach a consensus on first-line therapy for AMH and whether or not therapeutic choices may change for different patient sub-groups.
The group of dermatologists found that most patients with acne and AMH would benefit from early and efficacious acne treatment using a topical retinoid and benzoyl peroxide. Furthermore, other therapies, such as hydroquinone, azelaic acid, chemical peel, or antioxidants, may also be considered in an effort to enhance the effect of the treatment regimen. They also agreed that chemical peels could be used as an adjunctive or second-line therapy.
Nada Elbuluk, MD, MSc, one of the expert dermatologists who took part in this Delphi consensus, will be presenting a session, Melasma and Post-Inflammatory Hyperpigmentation: How to Prevent and How to Treat, at the upcoming SBS: West Coast Derm in Southern California. Don’t miss out on the opportunity to learn more about this condition and how to better care for your patients with PIH.
Register now for SBS: West Coast Derm taking place this coming Oct. 6-7, 2023.
















